Do you or anyone you know suffer from lower back pain? It is one of the most common orthopedic presentations that we see in the clinic. Statistics show that the percentage of adults with back pain increases with age, from 28.4% for those aged 18–29 and 35.2% for those aged 30–44 to 44.3% for those aged 45–64 and 45.6% for those aged 65 and over. The disc is one of the most common culprits, particularly in recurrent pain. Since your spine is the center of everything you do, these injuries can range from mildly limiting to affecting even the most simple tasks of daily life.
What are the discs?
The spine is made up of 24 bones. The discs are the tissue located in between each vertebra. Commonly referred to as the intervertebral discs, they function primarily to allow movement between adjacent vertebral bodies, absorb shock, and transmit loads through the vertebral column.
Disc Anatomy:
Before we explain the different types of problems people can have with their discs, it is essential to understand the anatomy of an intervertebral disc.
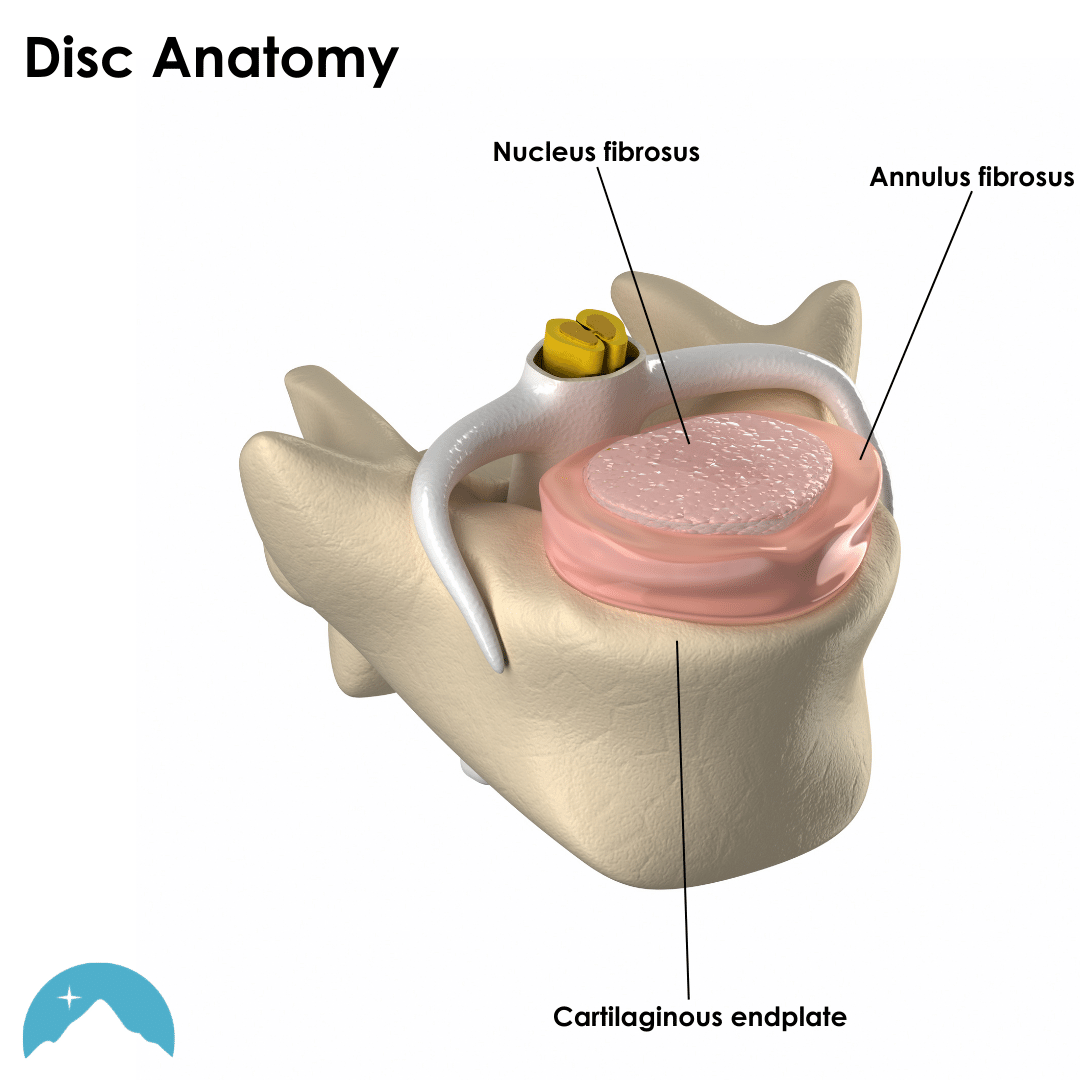
Each disc has three major components: the inner or nucleus pulposus (NP), the outer or annulus fibrosus (AF), and the cartilaginous endplates that anchor the discs to adjacent vertebrae. The nucleus is a gel-like structure that sits at the center of the intervertebral disc. It accounts for much of the strength and flexibility of the spine, along with load distribution. The annulus is a group of ring-shaped fibrous connective tissues called “lamellae” that surround the nucleus and function to support it.
What causes disc pathology?
Over time, an acute injury, movement imbalance, or repeated trauma can lead to disc problems. These can present as “contained” pathologies, such as disc sensitivity, annular tearing, or a bulging disc. In each of these cases, the supporting annular rings are intact and functioning to support the nucleus material.
The disc can also herniate, which occurs when disc material is pushed out of the annulus into the spinal canal through a tear or rupture. In this case, the material is no longer contained and can lead to trauma to the surrounding nerve roots. In severe cases, the herniated material breaks off, causing a free fragment to float in the canal. This is called a sequestered disc.
What are the signs of disc pain?
Disc pain can be highly variable and range from minor discomfort to severe pain affecting the peripheral nerves of your extremities or spinal cord. Signs of disc pain frequently present as:
- Morning pain/stiffness
- Pain with bending/rotation/lifting
- Pain with extended sitting/transitioning from sitting
- Pain in the extremities (arm pain or sciatic pain)
- Numbness/tingling
- A feeling of weakness in the arms/hands or legs
- Pain with cough/sneezing
- Repeated episodes of acute low back pain
When to seek medical attention:
Acute pain with weakness, severe/unrelenting pain, or signs of bowel and bladder dysfunction are all reasons to seek immediate care. Any bowel and bladder symptoms can be a medical emergency and require special attention for appropriate treatment. Fortunately, most disc pathology is treatable and will go away in time when managed appropriately, even herniated discs. Healing time varies from a few days to weeks or months. If symptoms last longer than six weeks or you suffer from recurrent episodes of pain, it is recommended that you seek care to assist in your recovery.
How physical therapy can help discogenic pain
Physical therapists are highly trained in evaluating and treating disc pathology. Treatment varies depending on your presentation. With acute injuries, we focus on education, posture, positional, and movement management to assist in guiding your body through the inflammation phase to reduce your recovery time. Pain relieving modalities may be used when indicated. Most importantly, we continue to assess if there is any need for further medical treatment, such as medication management or imaging and communicate this with your referring doctor or specialist. As the initial acute symptoms resolve, physical therapy focuses on short-term strategies for restoring movement and function and long-term strategies for preventing recurrence.
Strength and exercise are integral to a successful recovery. Current medical research supports movement and targeted exercise as effective long-term solutions for neck and back pain. Knowing what to do for your condition versus a general exercise program can differentiate between healing and developing persistent pain.
If you’re struggling with pain, we can help. Through an evaluation consisting of a detailed medical history and neurologic and movement assessment, our therapists can identify causative factors, provide treatment prognosis, and plan an active recovery that leads to a long-term solution for you! If interested, contact the spine care experts at Alpine at 541-382-5500.
